Painful Frozen Shoulder? Ouch! An Expert’s Guide
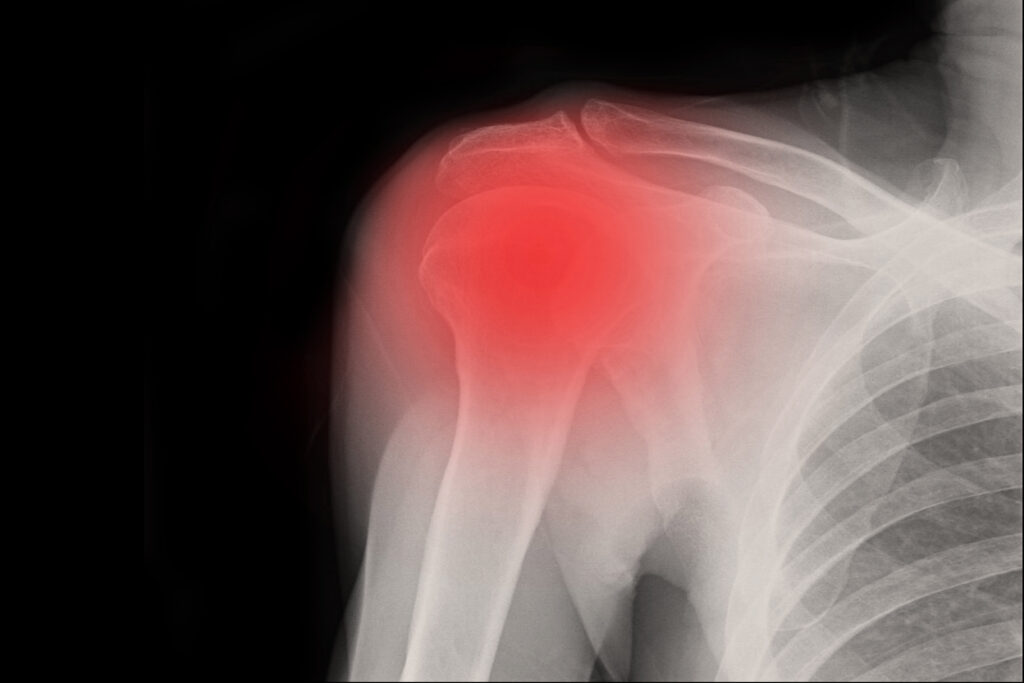
The pain of a frozen shoulder can be excruciating, and can make life a misery. Even tasks as simple as lifting a bag, hitting a tennis ball or rolling over in bed can become moments of intense pain, and sufferers often describe a sensation of feeling like their shoulder is ‘ripping’. But what actually is a frozen shoulder and how does it happen? Here, London-based Consultant Orthopaedic Surgeon, Carlos Cobiella, reveals everything you should know about this common ailment.
What is a frozen shoulder?
A frozen shoulder is a condition – not an injury. “We don’t know quite what triggers a frozen shoulder although it will often follow an injury,” says Carlos who has treated many well-known A-list Oscar winning actors and directors and some of the world’s top professional sportsmen and athletes. “However, a frozen shoulder is more common in people that suffer from diabetes or Dupuytren’s disease (where they have fibrous bands in the hands), and tends to happen in people between the ages of 40 and 60. In Japan it is referred to as ‘the 50-year-old shoulder’, however it can happen at any age.”
In Japan it is referred to as ‘the 50-year-old shoulder’
How does it happen?
“The condition usually starts as a niggling discomfort that gets worse progressively, and then a sharp pain in the shoulder on a sudden movement,” says Carlos. ”This is usually followed by progressive pain that starts interfering with sleep and daily chores and activities. Simple tasks such as carrying the shopping or walking the dog start to become painful and restricted, and the condition can gradually take its toll on the quality of life.”
Carlos, who specialises in upper limb and sports injuries, continues, “A frozen shoulder happens when the tissue around your shoulder joint becomes inflamed. The tissue then gets thickened, irritated, tighter and shrinks, which causes pain. A frozen shoulder can take at least one and a half to three years to get better and sometimes it can be longer and will go through three phases. Firstly, the initial acute phase of intense pain, then followed by the improvement of pain but restriction of movement, and then finally the resolution phase, when the symptoms settle progressively. However, it is quite common for the disease not to behave in this way, but to remain painful as well as restricted for a long time.”
How is it diagnosed and treated?
“When I have a patient with a frozen shoulder I assess their restriction of movement in all directions, if there is any indication of restriction no matter how mild, this calls for further investigation. Similar restrictions can often be caused by arthritis, or in very rare cases tumours, and so it is important to do imaging testing to rule out these other conditions and to confirm the diagnosis.
“We do not have a cure for frozen shoulders, but we can find a way to manage the symptoms in the short term, which are mostly pain and/or lack of mobility. It’s important that patients understand that the pain they are feeling is not damage – it is simply the shoulder joint tissue which has become irritated, and (similar to an infection), and any movement that stretches it might cause pain, but will not cause any damage to the joint. Therefore a patient should be able to live with the condition and although they may have pain on a daily basis, it will not be causing damage to the joint.
“Physiotherapy in the form of stretching exercises generally has a limited role, yet when moving from the initial acute pain to the restricted phase, it can help regain some movement. Massage can also help relieve the secondary pain that appears over the trapezius area for a few days and it can also be very helpful at the end of the process, during the resolution phase. After a while the muscles around the shoulder will be weak and so a gentle targeted exercise program can help restore normality.
“Cortisone injections into the main ball and socket joint (usually image guided as the joint is very difficult to inject blindly) can help relieve the pain. They do not have a direct effect on the tightness of the capsule, but patients usually get better function as they can use their shoulder with less or no pain, and they can sleep as they can lie on it and doesn’t wake them up. Cortisone injections can sometimes last for the duration of the condition, or may wear off after a few months. Repeating the injections at 3-4 months intervals is possible and there is no evidence that this causes any harm to the joint or the tendons.
“Surgery can be done on a frozen shoulder with an arthroscopy or keyhole procedure, and can be done as a day case, with the patient awake under local anaesthetic. For patients that do not want to know what is happening, sedation or a light general anaesthetic can be added. The procedure is usually done in a very short period of time, 10 to 15 minutes, and consists of cutting and removing the thickened and inflamed tissue. It is followed by a very gentle manipulation to release the final strands of tight tissue. The patient will generally go home the same day and start using their arm as soon as the local anaesthetic block wears off. The first two or three days are quite uncomfortable and you’ll need painkillers and ice, but progressively the patient can use their arm for general daily living. After that initial painful phase they can start doing gentle mobilisation exercises under the care of a physiotherapist for three or four weeks, until the movement range stabilises.
“None of these interventions will cure a frozen shoulder, but they will give a much better quality of life, until the frozen shoulder resolves itself. In summary, this is a condition that does not affect health, but can have a great impact on quality of life. It does settle on its own, but takes a couple of years to do so. While it lasts there are certain things that can make daily life much more pleasant.”