Dr Philippa Kaye On Allergies

Dr Philippa Kaye explains the many different allergies people can suffer from – and how to deal with a serious reaction…
Melody had eczema, asthma and hayfever but recently she thought something else was going on. A few times she had been out for a meal and noticed that her mouth was tingly and sore.
Then she ate a salad and not only did her mouth and tongue get sore but they felt swollen, as did her eyes.
She wanted to know what it could be, though by the time she came to see me her symptoms had resolved entirely. After taking a history as usual I said I thought this was an allergy.
Melody was initially confused as she knew hayfever was an allergy to pollen but that made her sneeze and her eyes itch, not her mouth swell. How could the treatment be the same?
I explained that an allergy occurs when the body’s immune system reacts to an agent which is harmless, such as food.
Seasonal and year-round allergies
There are lots of types of allergy. Your doctor will always ask if you are allergic to any medication, but you can also be allergic to food, plants, animal dander, even house dust mites.
Some allergies will be seasonal, such as hayfever – an allergy to grass or tree pollens, and some will be year-round, such as house dust mite allergy. You get an allergic reaction when exposed to an allergen, the thing to which you are allergic. So if you are allergic to a food, animal sting or medication you will only get the reaction when they get into your body.
Allergy symptoms
Some allergens will give respiratory symptoms such as runny nose, sneezing or itchy, runny eyes – for example house dust mite allergy, hayfever or animal dander allergy. Others will give a rash, mouth or tongue swelling or tingling and eye swelling, such as a drug or food allergy.
How are allergies diagnosed?
Blood tests can be used to diagnose allergies, as can skin patch tests, where a grid is marked onto the skin and drops of a fluid containing an allergen rubbed into tiny pricks in the skin to see if a skin reaction occurs. If you’re referred for these do not take an antihistamine beforehand; it will interfere with the results.
How are allergies treated?
The mainstay of treatment for allergies is oral antihistamines. These can be effective for all allergies. Other treatments will then depend on your symptoms. For example, for hayfever if you have itchy, watery eyes you may be offered eye drops, for a runny nose and sneezing, a steroid nasal spray may help and if you get a tight chest and wheezing you may require inhalers.
Treatments for an allergic reaction to a food or medication will also include an oral antihistamine but if there is anaphylaxis you may also be given oral or intravenous steroid medication. Depending on the severity of your allergy, you may be prescribed an adrenaline auto-injector in case of anaphylaxis. If you have to use your adrenaline autoinjector, such as an Epipen, Jext or Emerade pen you should always seek urgent medical advice.
What is anaphylaxis?
Allergies can lead to anaphylaxis, a potentially catastrophic medical emergency. Symptoms include swelling, difficulties breathing and palpitations. If this happens, please phone 999 for an ambulance.
If at all possible you should avoid your allergen. So if you are allergic to nuts you don’t eat anything that could contain nuts, or traces of nuts. There is labelling on all manufactured foods to include allergens.
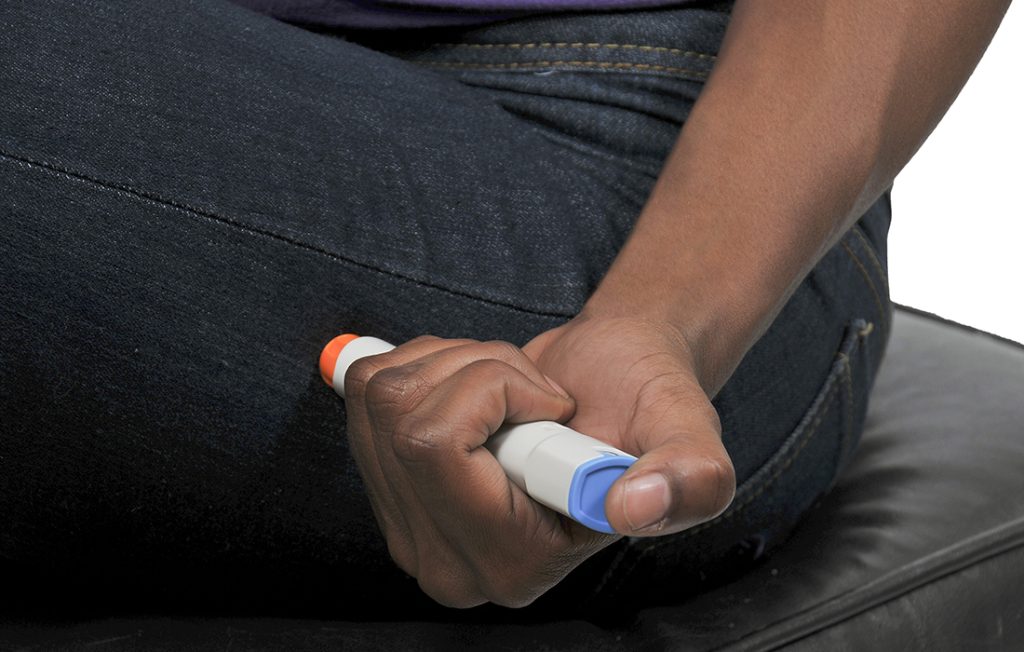
How to use an adrenaline auto-injector
If you are prescribed an adrenaline auto-injector you will be taught to use it in the following way:
- Once removed from the container and uncapped, the pens will inject when pressed firmly against the body.
- Hold the pen in the middle, in case you are holding it upside down.
- You do not need to remove clothing. Hold the pen firmly against the leg and you should hear a click as it auto-injects. Hold in place for 3 seconds.
- Remove the pen and the needle will automatically be capped.
- Seek urgent medical assistance.
Advice given in this article and on the My Weekly website and magazines is not meant to replace personalised medical advice from your doctor. If you have any health concerns please see your doctor.
Article written on August 6, 2020; article reviewed and updated on April 19, 2024
Each week we’ll ask Dr Philippa Kaye to talk about a prominent health issue, so look out for more articles in our health and wellbeing section in coming weeks. Read her advice on Parkinson’s Disease, Shingles, Ovarian Cancer, Endometriosis, Long Covid, Ticks and Lyme Disease and Eating Disorders.